Treatment for Cervical and Thoracic Spondylosis

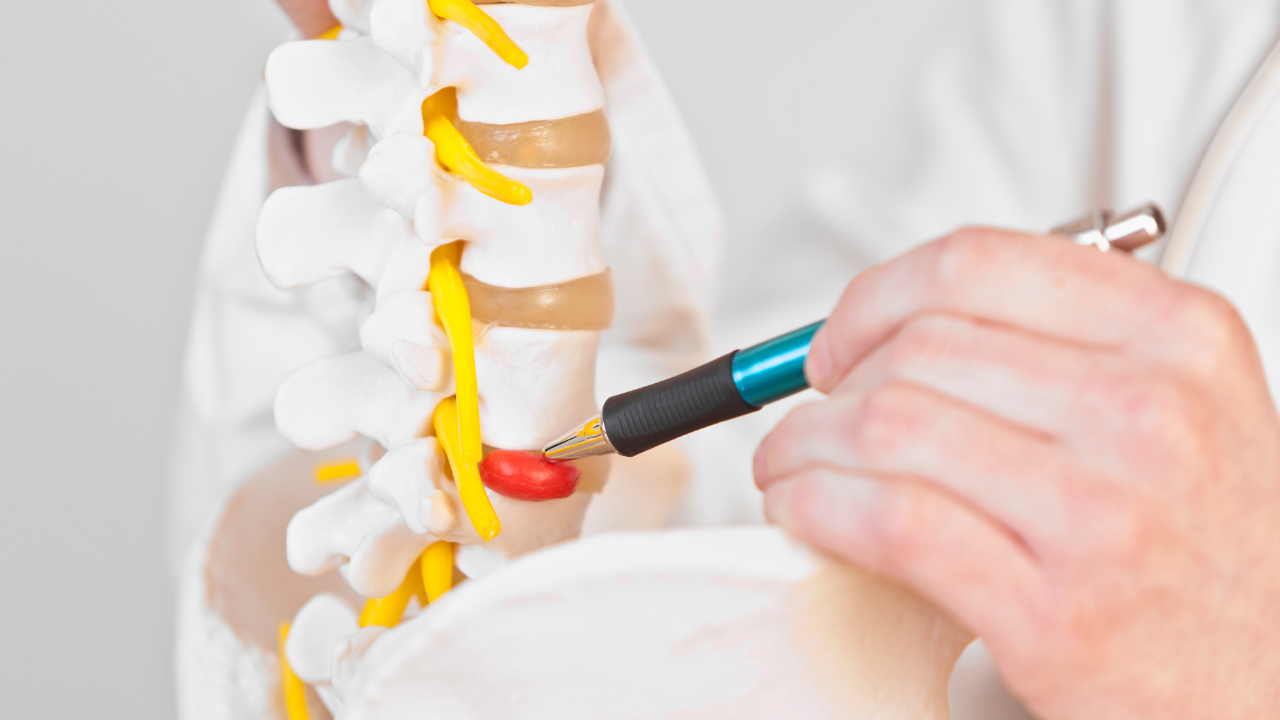
Trigger points may have an impact on the development and severity of cervical spondylosis
Spondylosis is a medical term for both osteoarthritis of the spine and the general wear and tear that occurs in the joints and bones of the spine as people age
The term can be used to describe degeneration in the neck—when this occurs it is referred to as cervical spondylosis. When it occurs in the middle back it is referred to as thoracic spondylosis.
Cervical Spondylosis
The most common symptoms of cervical spondylosis are neck pain, stiffness, and headaches. There may be a headache that originates in the neck, shoulder, arms, or chest, and a grinding noise or sensation when the neck is turned.
Symptoms of cervical spondylosis tend to improve with rest. Symptoms are generally most severe in the morning and again at the end of the day.
As we age, the discs of the cervical spine in the neck gradually break down, lose fluid, and become stiffer. From age 50 onward, the discs between the vertebrae become less spongy and provide less of a cushion.
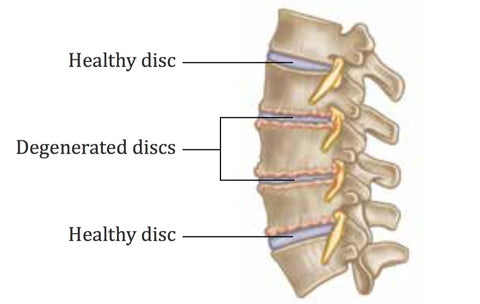
Bones and ligaments get thicker, encroaching on the space of the spinal canal. By the time they reach their 60s, around 90% of the population will have some degree of cervical spondylosis.
Posture, employment, lifestyle choices, and certain exercise regimes can also have an impact on the development and severity of cervical spondylosis.
If cervical spondylosis results in pressure on the spinal cord (cervical stenosis), it can damage nerves—a condition called cervical myelopathy— leading to pain and/or pins and needles in the arms and legs, a loss of feeling in the hands and legs, a loss of coordination and difficulty walking, muscle spasms, and abnormal reflexes.
Cervical spondylosis is usually diagnosed through a physical examination, X rays, CT scans, and MRI. Most problems caused by cervical spondylosis will settle down, although they may reoccur at a later stage.
Treatment
Treatment may include the use of nonsteroidal anti-inflammatory drugs, corticosteroid injections, the short-term use of cervical collars, physiotherapy or chiropractic treatment, hot and cold therapy, exercise, and firm pillow support.
In a small number of cases where conservative treatments have failed then surgery may be recommended, and in around one in ten cases a person can go on to develop long-term (chronic) neck pain.
Thoracic Spondylosis
As the thoracic spine doesn’t work as hard as the lumbar or cervical spine, degeneration tends to begin elsewhere before affecting the thoracic spine.
However, this is not always the case, as spondylosis can affect any part of the spine.
Common symptoms of thoracic spondylosis include: pain and stiffness in the mid-back, particularly in the morning after getting out of bed; tingling or numbness in the legs, arms, hands, or feet; muscle weakness; and a loss of coordination or difficulty walking.
For cases of thoracic spondylosis, treatment is usually conservative. Rest, lifestyle or work-habit changes, pain-relieving medications, physiotherapy, chiropractic or acupuncture treatments, and trigger point therapy are usually effective.
Only in the most severe cases would surgery be indicated.
Trigger Point Therapy
Trigger point therapy can help in reducing pain, to allow the muscles to settle back to normal functioning, and to prevent the problem spreading to other areas as the client stiffens up in response to pain and overcompensates by using a different set of muscles.
In cases of cervical spondylosis we usually look to treat trigger points in the upper trapezius, levator scapulae, semispinalis capitis, splenius cervicis, and sub-occipital muscles.
For thoracic spondylosis we look at levator scapulae, serratus anterior, infraspinatus, rhomboids, multifidi, latissimus dorsi, scalenes, and rectus abdominis.
Trigger point therapy should target the natural "holding patterns" that the body will trigger in response the injury.
This will often address the stiffness issues and provide increased and less painful range of motion.
Links
Find a Trigger Point Professional in your area
More Articles About Trigger Points
More Articles About Frozen Shoulder
More Articles About Shoulder Pain
Certify as a Trigger Point Therapist
About NAT Courses
As a manual therapist or exercise professional, there is only one way to expand your business - education!
Learning more skills increases the services that you offer and provides more opportunity for specialization.
Every NAT course is designed to build on what you already know, to empower you to treat more clients and grow your practice, with a minimal investment in time and money.
Help Desk
About Niel Asher Education
Niel Asher Education is a leading provider of distance learning and continued education courses.
Established in the United Kingdom in 1999, we provide course and distance learning material for therapists and other healthcare professionals in over 40 countries.
Our courses are accredited by over 90 professional associations and national accreditation institutions including the National Academy of Sports Medicine (NASM) and National Certification Board for Therapeutic Massage and Bodywork (NCBTMB). Full details of all international course accreditations can be found on our website.
Printed course materials and other products offered on our websites are despatched worldwide from our 3 locations in the UK (London), USA (Pennsylvania) and Australia (Melbourne).
More About Us
NAMTPT AWARD
We are honored to have received the "Excellence in Education" Award from the National Association of Myofascial Trigger Point Therapists.
Since 1999 Niel Asher Education has won numerous awards for education and in particular for education and services provided in the field of trigger point therapy.
Read Full Article
Award Winning Instructors
Niel Asher Healthcare course instructors have won a host of prestigious awards including 2 lifetime achievement honorees - Stuart Hinds, Lifetime Achievement Honoree, AAMT, 2015, and Dr. Jonathan Kuttner, MD, Lifetime Achievement Honoree, NAMTPT, 2014.
Meet the Instructors
Accreditation

If you are a qualified/licensed manual therapist or exercise/fitness professional you can expand your credentials with NAT certification.
In addition to national accreditation for continued education, each course that we offer includes "NAT Learning Credits". By taking and completing courses you can accumulate NAT credits to qualify for NAT certification.
There are currently 3 levels of NAT certification. Certifying NAT is a valuable way to show your clients that you take continued education seriously, and to promote your skills and qualifications.
Most of our courses are accredited for CE/CPD/CPE. A full list of CE accreditations can be found by clicking on the link below.
About NAT Certification
Niel Asher Technique
Since 1999 the Niel Asher Technique for treating trigger points has been adopted by over 100,000 therapists worldwide, and has been applied to the treatment of a number of common musculoskeletal injuries.
The Niel Asher Technique for treating frozen shoulder was first introduced and published in 1997 and has been widely adopted by therapists and exercise professionals working within elite sports and athletics.
Read More
International Students
Most of our courses are available as either "Printed" or 'Download" editions, wherever you live. Internet connection is required to access online and downloadable material.
When you purchase a download edition, you receive immediate lifetime access to all course material. Course texts can be downloaded and printed if required.
When you purchase a "Printed" edition, you will also receive free access to the download edition.
We ship Worldwide from locations in the USA, UK, and Australia. Most items are despatched within 24 hours and shipping is FREE for all orders over US$50.
Shipping
Where to Start?
We offer a range of over 50 courses, presented by some of the worlds leading manual therapists. All courses are reviewed annually, and new courses are regularly added.
Our courses are modular, and designed to build on what you already know. For more information, please visit our "Where to Start?" page.
Start Here
Trigger Point Therapy Master Course

Learn More for Less
Unlimited access to all courses for just $19.95/mo