Trigger Point Therapy - Treating the Hip Adductors
Treating the hip adductors - Stuart Hinds
The adductor magnus is the largest of the adductor muscle group, which also includes the adductor brevis and adductor longus.
The adductor longus is the most anterior of the three. The adductor brevis lies anterior to the adductor magnus.
The lateral border of the upper fibers of the adductor longus form the medial border of the femoral triangle (the sartorius forms the lateral boundary; the inguinal ligament forms the superior boundary).

Adductor Magnus - Common Trigger Point Sites

Adductor Brevis and Adductor Longus - Common Trigger Point Sites
ORIGIN
Anterior part of pubic bone (ramus). Adductor magnus also takes origin from ischial tuberosity.
INSERTION
Whole length of medial side of femur, from hip to knee.
ACTION
Adduct and laterally rotate hip joint. Adductors longus/brevis also flex extended femur and extend flexed femur.
NERVE
Magnus: posterior division of obturator nerve L2, 3, 4. Tibial portion of sciatic nerve, L4, 5, S1. Brevis: anterior division of obturator nerve, (L2–L4). Sometimes the posterior division also supplies a branch to it.
Longus: anterior division of obturator nerve, L2, 3, 4.
BASIC FUNCTIONAL MOVEMENT
Example: bringing second leg in or out of a car.

REFERRED PAIN PATTERNS
There are several zones of referred pain: (1) two zones localized around anterior hip 5–8 cm, and above knee 5–8 cm; (2) whole anteromedial thigh from inguinal ligament to medial knee joint; (3) medial thigh from hip to knee.

INDICATIONS
Deep pain/tenderness in medial thigh, hip/leg stiffness on abduction, pain on weight bearing/rotating hip, “clicky” hip, hot/stinging pain under thigh, groin strain, post hip- replacement/fracture rehabilitation, renal tubular acidosis, swollen legs, osteoarthritis of hip.
CAUSES
Leg splint/cast, foot/ankle problems, sudden overload due to gymnastics, football/ice skating injury, horse riding, skiing, cross-legged sitting.
DIFFERENTIAL DIAGNOSIS
Avulsion. Pubic symphysis dysfunction. Neuropathy. Lymphadenopathy. Hernia. Knee pain (mechanical). Osteoarthritic hip. Femoral herniation.
CONNECTIONS
Pectineus, vastus medialis, iliopsoas, vastus lateralis, sartorius (lower end).
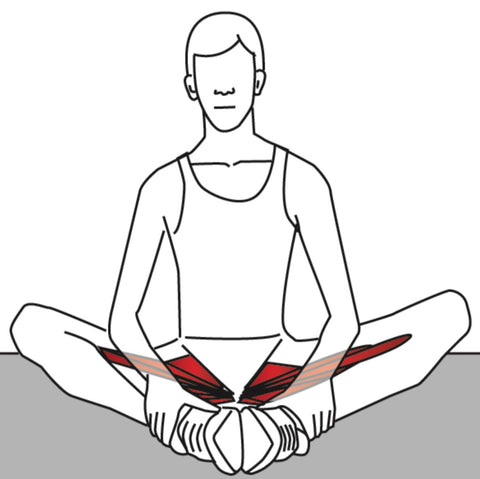
Prescribed stretching exercises can be useful
GENERAL ADVICE TO CLIENTS
Modify activities until trigger points diminish. Home stretch program. Avoid overuse at gym. Explore habitual postures. Check techniques (ex. skiing/ cycling). Explore vitamin/mineral deficiency.
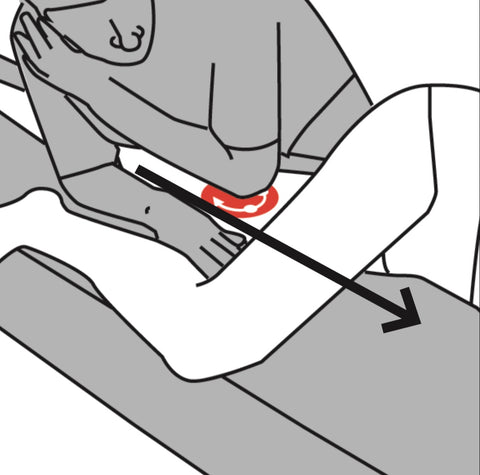
Treatment techniques include deep stroking massage, compression, muscle energy techniques, and positional release techniques
Post-Isometric (PIR) Technique
Indications: subacute to chronic settings
1. Identify the trigger point.
3. Using 10–25% of their power, ask the patient to contract the affected/host muscle at its maximal pain-free length, while applying isometric resistance for 3–10 seconds; stabilize the body part to prevent muscle shortening.
5. During this relaxation phase, gently lengthen the muscle by taking up the slack to the point of resistance (passive)—note any changes in length.
Links
Find a Trigger Point Professional in your area
Corrective Exercises for Hip and Shoulder
Treating Hip Pain and Dysfunction
Certify as a Trigger Point Therapist
About NAT Courses
As a manual therapist or exercise professional, there is only one way to expand your business - education!
Learning more skills increases the services that you offer and provides more opportunity for specialization.
Every NAT course is designed to build on what you already know, to empower you to treat more clients and grow your practice, with a minimal investment in time and money.
Help Desk
About Niel Asher Education
Niel Asher Education is a leading provider of distance learning and continued education courses.
Established in the United Kingdom in 1999, we provide course and distance learning material for therapists and other healthcare professionals in over 40 countries.
Our courses are accredited by over 90 professional associations and national accreditation institutions including the National Academy of Sports Medicine (NASM) and National Certification Board for Therapeutic Massage and Bodywork (NCBTMB). Full details of all international course accreditations can be found on our website.
Printed course materials and other products offered on our websites are despatched worldwide from our 3 locations in the UK (London), USA (Pennsylvania) and Australia (Melbourne).
More About Us
NAMTPT AWARD
We are honored to have received the "Excellence in Education" Award from the National Association of Myofascial Trigger Point Therapists.
Since 1999 Niel Asher Education has won numerous awards for education and in particular for education and services provided in the field of trigger point therapy.
Read Full Article
Award Winning Instructors
Niel Asher Healthcare course instructors have won a host of prestigious awards including 2 lifetime achievement honorees - Stuart Hinds, Lifetime Achievement Honoree, AAMT, 2015, and Dr. Jonathan Kuttner, MD, Lifetime Achievement Honoree, NAMTPT, 2014.
Meet the Instructors
Accreditation

If you are a qualified/licensed manual therapist or exercise/fitness professional you can expand your credentials with NAT certification.
In addition to national accreditation for continued education, each course that we offer includes "NAT Learning Credits". By taking and completing courses you can accumulate NAT credits to qualify for NAT certification.
There are currently 3 levels of NAT certification. Certifying NAT is a valuable way to show your clients that you take continued education seriously, and to promote your skills and qualifications.
Most of our courses are accredited for CE/CPD/CPE. A full list of CE accreditations can be found by clicking on the link below.
About NAT Certification
Niel Asher Technique
Since 1999 the Niel Asher Technique for treating trigger points has been adopted by over 100,000 therapists worldwide, and has been applied to the treatment of a number of common musculoskeletal injuries.
The Niel Asher Technique for treating frozen shoulder was first introduced and published in 1997 and has been widely adopted by therapists and exercise professionals working within elite sports and athletics.
Read More
International Students
Most of our courses are available as either "Printed" or 'Download" editions, wherever you live. Internet connection is required to access online and downloadable material.
When you purchase a download edition, you receive immediate lifetime access to all course material. Course texts can be downloaded and printed if required.
When you purchase a "Printed" edition, you will also receive free access to the download edition.
We ship Worldwide from locations in the USA, UK, and Australia. Most items are despatched within 24 hours and shipping is FREE for all orders over US$50.
Shipping
Where to Start?
We offer a range of over 50 courses, presented by some of the worlds leading manual therapists. All courses are reviewed annually, and new courses are regularly added.
Our courses are modular, and designed to build on what you already know. For more information, please visit our "Where to Start?" page.
Start Here





This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.
About Niel Asher Education
Niel Asher Education (NAT Global Campus) is a globally recognised provider of high-quality professional learning for hands-on health and movement practitioners. Through an extensive catalogue of expert-led online courses, NAT delivers continuing education for massage therapists, supporting both newly qualified and highly experienced professionals with practical, clinically relevant training designed for real-world practice.
Beyond massage therapy, Niel Asher Education offers comprehensive continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals working across a wide range of clinical, sports, and wellness environments. Courses span manual therapy, movement, rehabilitation, pain management, integrative therapies, and practitioner self-care, with content presented by respected educators and clinicians from around the world.
Known for its high production values and practitioner-focused approach, Niel Asher Education emphasises clarity, practical application, and professional integrity. Its online learning model allows practitioners to study at their own pace while earning recognised certificates and maintaining ongoing professional development requirements, making continuing education accessible regardless of location or schedule.
Through partnerships with leading educational platforms and organisations worldwide, Niel Asher Education continues to expand access to trusted, high-quality continuing education for massage therapists, continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals, supporting lifelong learning and professional excellence across the global therapy community.

Continuing Professional Education
Looking for Massage Therapy CEUs, PT and ATC continuing education, chiropractic CE, or advanced manual therapy training? Explore our evidence-based online courses designed for hands-on professionals.




















