Trigger Point Therapy - Masseter
Ischemic Compression Technique
Masseter trigger points are significant contributors to headaches
A forward-head posture places the mandible in a position that puts the masseter under undue stress.
Antagonist muscles, such as the geniohyoid, omohyoid, and digastric, can all become spastic as a result of overtraining of the abdominal muscles using poor technique.
This in turn may inhibit the masseter, with resulting trigger point formation to provide stiffness or tension within the muscle.
Changes in associated suboccipital muscles lead to changes in homeostasis of the head and face muscles.
A change in the positioning of the temporomandibular joint will also affect the position of the cervical spine.
Correct alignment of the temporomandibular joint requires treatment of the masseter and pterygoids at the local level, with attention to core efficiency at the global level.
The masseter is a complex muscle, and pain is referred into the eyebrow, maxilla, mandible (anterior), and upper and lower molar teeth.
Any person with a toothache will rightly go to a dentist.
With no obvious pathology presenting, it is in the patient’s best interests to rule out the possibility of referred pain from trigger points being at the root of the pain.
Other related sensations include hypersensitivity to pressure and temperature changes (e.g. during flights).
Pain and changes in sensations can also refer into the temporomandibular joint and inner ear.
Remember also that masseter trigger points are significant contributors to headaches.
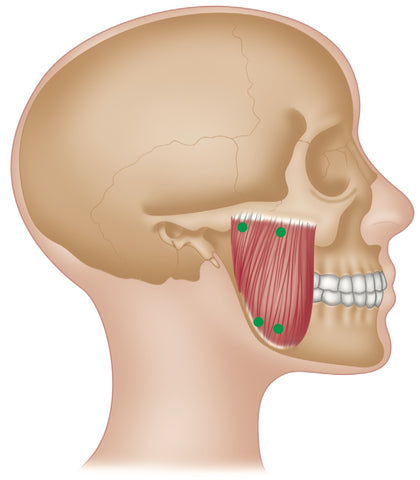
Masseter - Common Trigger Point Sites
Origin
Zygomatic process of maxilla. Medial and inferior surfaces of zygomatic arch.
Insertion
Angle of ramus of mandible. Coronoid process of mandible.
Action
Closes jaw. Clenches teeth. Assists in side to side movement of mandible.
Antagonist: platysma.
Nerve
Trigeminal V nerve (mandibular division).
Basic Functional Movement
Chewing food.
Referred Pain Patterns
Superficial: eyebrow, maxilla, and mandible (anterior). Upper and lower molar teeth.
Deep: ear and TMJ.
Indications
Trismus (severely restricted jaw), TMJ pain, tension/stress headache, ear pain, ipsilateral tinnitus, dental pain, bruxism, sinusitis pain, puffiness under the eyes (often present in singers).
Causes
Chewing gum, tooth grinding/ bruxism, prolonged dental work, stress, emotional tension, head- forward postures.
Differential Diagnosis
TMJ pain/syndrome. Tinnitus. Trismus.
Connections
Ipsilateral temporalis, medial pterygoid, contralateral masseter, SCM.
Trigger Point Treatment Techniques
| Compression | YES |
| Muscle Energy Techniques | YES |
| Positional Release | YES |
| Dry Needling | YES |
Bite Plates/Occlusal Splints
Opinion varies as to efficacy, type, and duration of use of occlusal devices. An evidence base suggests they can be beneficial.
Breathing and Stress Control Techniques
Stress, tension, and poor breathing mechanics can be a factor. Autogenic and breathing methods might be worth exploring for some.
Posture
Head forward or upper crossover patterns can be treated by a range of manual and trigger point therapists.
Advice
Stop tooth grinding (bite plates). Work posture (telephone). Posture of head–neck–tongue. Stop chewing gum/ice/nails.
Self Help
Use pincer grip, placing thumb inside the mouth.
Links
Find a Trigger Point Professional in your area
More About Ischemic Compression Technique
Dry Needling for Trigger Points
Certify as a Trigger Point Therapist
About NAT Courses
As a manual therapist or exercise professional, there is only one way to expand your business - education!
Learning more skills increases the services that you offer and provides more opportunity for specialization.
Every NAT course is designed to build on what you already know, to empower you to treat more clients and grow your practice, with a minimal investment in time and money.
Help Desk
About Niel Asher Education
Niel Asher Education is a leading provider of distance learning and continued education courses.
Established in the United Kingdom in 1999, we provide course and distance learning material for therapists and other healthcare professionals in over 40 countries.
Our courses are accredited by over 90 professional associations and national accreditation institutions including the National Academy of Sports Medicine (NASM) and National Certification Board for Therapeutic Massage and Bodywork (NCBTMB). Full details of all international course accreditations can be found on our website.
Printed course materials and other products offered on our websites are despatched worldwide from our 3 locations in the UK (London), USA (Pennsylvania) and Australia (Melbourne).
More About Us
NAMTPT AWARD
We are honored to have received the 2017 "Excellence in Education" Award from the National Association of Myofascial Trigger Point Therapists.
Since 1999 Niel Asher Education has won numerous awards for education and in particular for education and services provided in the field of trigger point therapy.
Read Full Article
Award Winning Instructors
Niel Asher Healthcare course instructors have won a host of prestigious awards including 2 lifetime achievement honorees - Stuart Hinds, Lifetime Achievement Honoree, AAMT, 2015, and Dr. Jonathan Kuttner, MD, Lifetime Achievement Honoree, NAMTPT, 2014.
Meet the Instructors
NAT Certification
If you are a qualified/licensed manual therapist or exercise/fitness professional you can expand your credentials with NAT certification.
In addition to national accreditation for continued education, each course that we offer includes "NAT Learning Credits". By taking and completing courses you can accumulate NAT credits to qualify for NAT certification.
There are currently 3 levels of NAT certification. Certifying NAT is a valuable way to show your clients that you take continued education seriously, and to promote your skills and qualifications.
About NAT Certification
Accreditation
NAT courses are accredited for continuing education by over 30 professional associations in North America, United Kingdom, Australia, and European Union countries. These include The National Academy of Sports Medicine, Physical Therapy Board of California, AAFA, National Certification Board for Manual Therapists and Bodyworkers, Sports Therapy Institute, and Myotherapy Australia.
See Full List
Niel Asher Technique
Since 1999 the Niel Asher Technique for treating trigger points has been adopted by over 100,000 therapists worldwide, and has been applied to the treatment of a number of common musculoskeletal injuries.
The Niel Asher Technique for treating frozen shoulder was first introduced and published in 1997 and has been widely adopted by therapists and exercise professionals working within elite sports and athletics.
Read More
International Students
Most of our courses are available as either "Printed" or 'Download" editions. When you purchase a download edition, you receive immediate lifetime access to all course material. Course texts can be downloaded and printed if required.
When you purchase a "Printed" edition, you will also receive free access to the download edition.
We ship Worldwide from locations in the USA, UK, and Australia. Most items are despatched within 24 hours and shipping is FREE for all orders over US$50.
Shipping
NEW RELEASE!
This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.
About Niel Asher Education
Niel Asher Education (NAT Global Campus) is a globally recognised provider of high-quality professional learning for hands-on health and movement practitioners. Through an extensive catalogue of expert-led online courses, NAT delivers continuing education for massage therapists, supporting both newly qualified and highly experienced professionals with practical, clinically relevant training designed for real-world practice.
Beyond massage therapy, Niel Asher Education offers comprehensive continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals working across a wide range of clinical, sports, and wellness environments. Courses span manual therapy, movement, rehabilitation, pain management, integrative therapies, and practitioner self-care, with content presented by respected educators and clinicians from around the world.
Known for its high production values and practitioner-focused approach, Niel Asher Education emphasises clarity, practical application, and professional integrity. Its online learning model allows practitioners to study at their own pace while earning recognised certificates and maintaining ongoing professional development requirements, making continuing education accessible regardless of location or schedule.
Through partnerships with leading educational platforms and organisations worldwide, Niel Asher Education continues to expand access to trusted, high-quality continuing education for massage therapists, continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals, supporting lifelong learning and professional excellence across the global therapy community.

Continuing Professional Education
Looking for Massage Therapy CEUs, PT and ATC continuing education, chiropractic CE, or advanced manual therapy training? Explore our evidence-based online courses designed for hands-on professionals.




















