Levator Ani Syndrome - Trigger Point Therapy Overview
Pelvic Pain and Levator Ani Syndrome - Dr. Jonathan Kuttner
If you have pelvic pain, chances are you have trigger points somewhere within or adjacent to your pelvic floor muscles
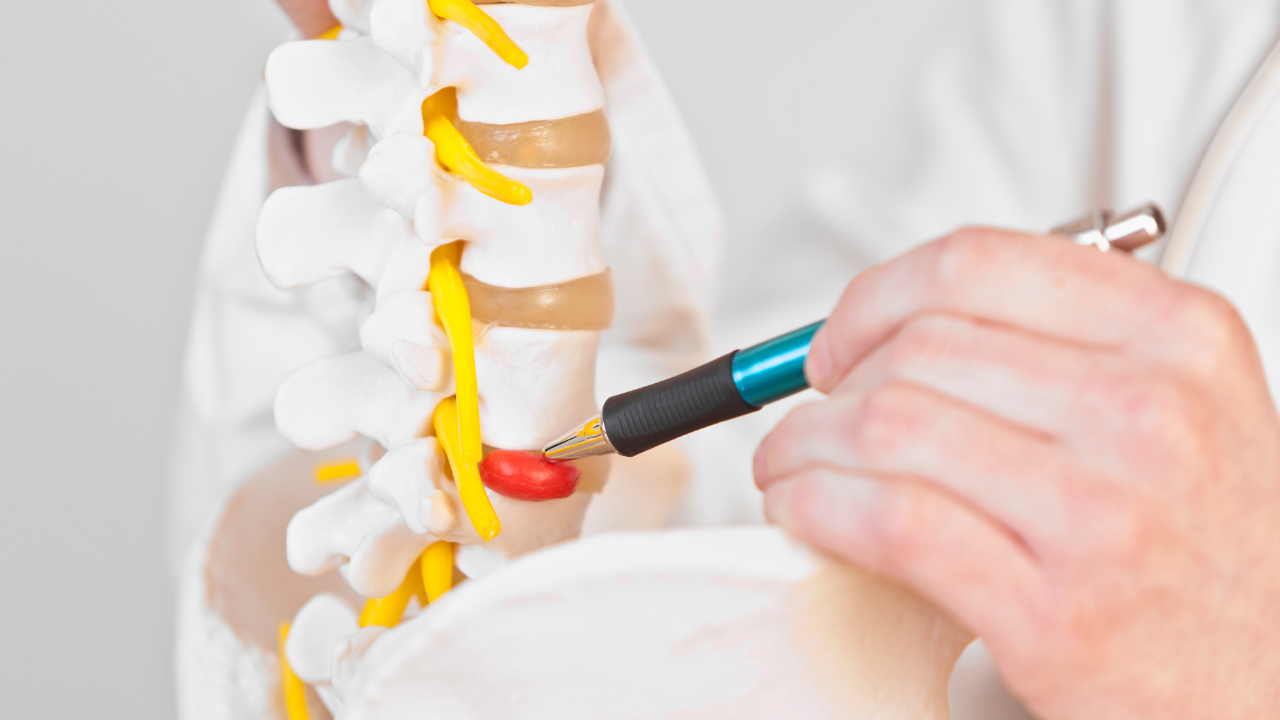
The levator ani consists of the pubococcygeus and the iliococcygeus muscles.
Together with the coccygeus muscle, these muscles form the pelvic diaphragm (the muscular floor of the pelvis).
We find that trigger points in the levator ani muscle are often implicated in low back pain, Levator Ani Syndrome, and a wide range of chronic pelvic pain syndromes.
Pelvic Disorders
Whilst trigger points may be the primary cause of pelvic pain in some patients; in others it may be a response to an underlying pelvic disorder.
There are many mechanisms of injury that can cause spasm of the pelvic floor. These include, but are not limited to:
Child birth injury, pelvic surgery, lumbar disc surgery, prolonged driving or occupations that require prolonged sitting, gait disturbances, pelvic inflammation or infection, traumatic injury to the back or pelvis, and injuries that result from sexual intercourse.
Malalignment of the Pelvis
Malalignment of the pelvis, especially in the sacroiliac joint, due to trauma, poor posture, muscular asymmetry, or excessive sports also may contribute to muscular dysfunction of the pelvis.

Levator Ani Syndrome
Levator Ani Syndrome is a condition in which the pelvic floor muscles, which provide support for the vagina, bladder and rectum, are in constant or frequent, muscle spasm and tightness.
This muscle spasm is often the body’s reaction to the pain produced by Vulvar Vestibulitis Syndrome or Prostatitis.
The muscle spasm can often last long after the initial cause of pain, and the muscle spasm itself can cause pain and restrict the blood supply to the damaged tissues.
Muscle Spasm
This muscle spasm is similar to the spasm and tension people often get in the neck and shoulder muscles, but in that case, you are often aware of the tension.
You can feel your muscles tightening and see the effect as your shoulders rise up above your neck.
This enables you to use techniques to reduce the tension, such as massage, exercises, relaxation techniques or just remind yourself to let go of the muscles.
However with the pelvic floor muscles, we are often unaware that they exist, let alone aware that they might be in spasm or particularly tight.
If we are unaware of the muscles, then we are unlikely to be able to relax them or reduce the tension in them.
Symptoms
Symptoms of Levator Ani Syndrome include:
- A dull ache in the rectum, vagina or perineum
- Constant rectal or vaginal pressure
- A constant burning in the rectum, vagina or perineum
- Feeling as though one is sitting on a ball or as though a ball is in the rectum
Passing feces often worsens symptoms and is difficult if you are experiencing Levator Ani Syndrome.
Sexual intercourse can also worsen your symptoms.
Levator Ani Syndrome is not thought to be psychological in origin; however, emotional stress may aggravate symptoms.
Treatment
Manual therapy is relatively successful for patients with chronic pain related to pelvic floor dysfunction, especially considering the typical outcome and persistence of symptoms for this patient population as a whole.
Only a few prospective randomized trials have been conducted, but FitzGerald et al demonstrated a 57% response rate to myofascial therapy for urologic pelvic pain syndrome among patients presenting with pelvic floor tenderness.
The same multi-center collaborative group later confirmed these results with a 59% response rate in women treated with myofascial therapy for interstitial cystitis and painful bladder syndrome.
Trigger Point Therapy
Weaving trigger point therapy into your treatment routines may have a profound effect.
Trigger points play a role in the vast majority of pelvic pain syndromes and in may cases they are the prime cause.
Patients should bear in mind that finding a therapist with the skill and interest to address pelvic floor dysfunction can be difficult in some geographical areas.
Do not attempt to perform these trigger point techniques unless they fall within your professional scope of practice.
Quick Links:
Find a Trigger Point Professional in your area
More About Pelvic Pain and Trigger Points
Dry Needling for Trigger Points
Certify as a Trigger Point Therapist
NAT Education Membership Plans - from $19.95/monthly


Online Education Plans for Massage and Manual Therapists
Unlimited Access to All NAT Courses and Certification Online
$19.95/monthly
This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.

Learn More for Less
Unlimited access to all courses for just $19.95/mo