Trigger Point Therapy - Raynaud’s Syndrome
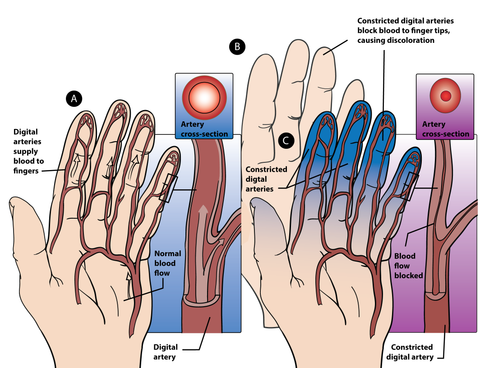
Renaud's Syndrome - Underlying Mechanism
Raynaud’s Syndrome is most commonly triggered by cold temperatures but it can also be triggered by anxiety or stress
With the onset of winter it's worth remembering that nasty (and surprisingly common) condition known as Reynaud's Syndrome. Depending on the climate in your region, there's every likelihood that you'll be seeing one or two cases of this in your practice over the coming weeks.
Reynaud's Syndrome
Raynaud’s syndrome, also known as Raynaud’s phenomenon, Raynaud’s disease, or simply Raynaud’s, is a condition that affects the blood supply to the extremities of the body.
The areas most frequently affected are the fingers and toes, but occasionally the earlobes, nose, nipples, or tongue can be affected. It is a common condition, more so in cold climates as cold is one of the prime triggers of an attack.
The fingers are the most commonly affected area, with an additional 40% of sufferers also experiencing symptoms in the toes. For ease, we will refer here to fingers but the same information and treatments apply to the toes.
Raynaud’s is a common problem, with up to 20% of the population affected in countries with colder climates. It affects more women than men and has a high hereditary factor, with the onset of symptoms usually coming before the age of 30.
Triggers and Symptoms
Raynaud’s is most commonly triggered by cold temperatures but it can also be triggered by anxiety or stress.
During an attack the digital arteries that supply the blood vessels in the fingers contract and blood flow is severely restricted.
At first the fingers go white and will feel very cool or cold to the touch. Then the fingers will go a blue as the oxygen from the blood in the narrowed blood vessels is quickly used.
Finally the fingers go bright red as the blood vessels reopen and the blood flow returns—at this stage the fingers may also throb, tingle, burn, or feel numb.
Attacks may last from a few minutes to several hours; for many people this is a mild and minor irritation that doesn’t have a significant impact on life, for others the symptoms will be more severe and there may need to lifestyle changes—for example, not working outdoors—to manage the condition.
There are medications available that can help,and these should be discussed by the sufferer with their doctor.
Primary and Secondary
There are two forms of Raynaud’s and the treatment given will depend on the form. More than 90% of sufferers have primary Raynaud’s.136 The cause of primary Raynaud’s is not known—it is not a symptom or part of another illness and symptoms completely disappear after each bout. Massage is very safe for people with primary Raynaud’s and self-massage can be applied when a bout occurs.
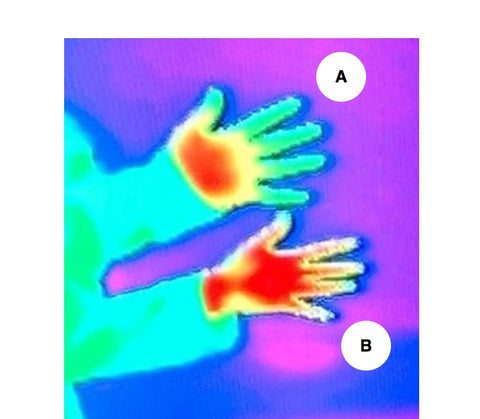
Image taken with a thermographic camera. Red shows warm areas whilst green indicates cool areas. "Reynaud's" hand (A). Healthy hand (B).
Secondary Raynaud’s occurs as a result of another condition or as a result of medication or injury. Most cases of secondary Raynaud’s are associated with autoimmune conditions, such as scleroderma (a condition that causes thickening and hardening of the skin), rheumatoid arthritis, Sjögren’s syndrome (a condition where the immune system attacks the body’s sweat and tear glands), lupus, or multiple sclerosis.
Some forms of cancer may also cause Raynaud’s, but secondary Raynaud’s does not always mean a severe underlying illness, as it can also be caused as a side effect of migraine medications, beta blockers, some decongestants, the contraceptive pill, or hormone replacement therapy.
When the Raynaud’s is secondary there will be other symptoms and onset is often much later in life; while primary Raynaud’s almost always affects all the fingers, secondary Raynaud’s symptoms may start with just one or two fingers. Secondary Raynaud’s always needs medical investigation so that the underlying cause can be diagnosed and treatment given.
Specific Contraindications
If the underlying cause of the condition has already been diagnosed then massage treatment can be given, using the precautions given for the underlying condition.
In rare cases there can be complications with secondary Raynaud’s with ulceration, infections, or in extreme cases gangrene. If there are any signs of damage, infection, or dead tissue (brown/black tissue that is shrinking) then immediate medical help should be sought and any massage would be very strongly contraindicated.
Massage and Trigger Point Treatments
The starting point for massaging someone with Raynaud’s is to make sure that your own hands are warm—for some people, being touched by cold hands would be enough to trigger an attack—and make sure that you pre-warm any massage oil that you might be using.
Treatment can be applied gently during an attack or more deeply between attacks.
Trigger Points
Myofascial trigger point (MTrP) nerve entrapment can worsen symptoms of Raynaud’s so check MTrPs associated with the referral patterns to the affected area.
Find a Trigger Point Professional in your area
Courses for Exercise Professionals
This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.
About Niel Asher Education
Niel Asher Education (NAT Global Campus) is a globally recognised provider of high-quality professional learning for hands-on health and movement practitioners. Through an extensive catalogue of expert-led online courses, NAT delivers continuing education for massage therapists, supporting both newly qualified and highly experienced professionals with practical, clinically relevant training designed for real-world practice.
Beyond massage therapy, Niel Asher Education offers comprehensive continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals working across a wide range of clinical, sports, and wellness environments. Courses span manual therapy, movement, rehabilitation, pain management, integrative therapies, and practitioner self-care, with content presented by respected educators and clinicians from around the world.
Known for its high production values and practitioner-focused approach, Niel Asher Education emphasises clarity, practical application, and professional integrity. Its online learning model allows practitioners to study at their own pace while earning recognised certificates and maintaining ongoing professional development requirements, making continuing education accessible regardless of location or schedule.
Through partnerships with leading educational platforms and organisations worldwide, Niel Asher Education continues to expand access to trusted, high-quality continuing education for massage therapists, continuing education for physical therapists, continuing education for athletic trainers, continuing education for chiropractors, and continuing education for rehabilitation professionals, supporting lifelong learning and professional excellence across the global therapy community.

Continuing Professional Education
Looking for Massage Therapy CEUs, PT and ATC continuing education, chiropractic CE, or advanced manual therapy training? Explore our evidence-based online courses designed for hands-on professionals.



















