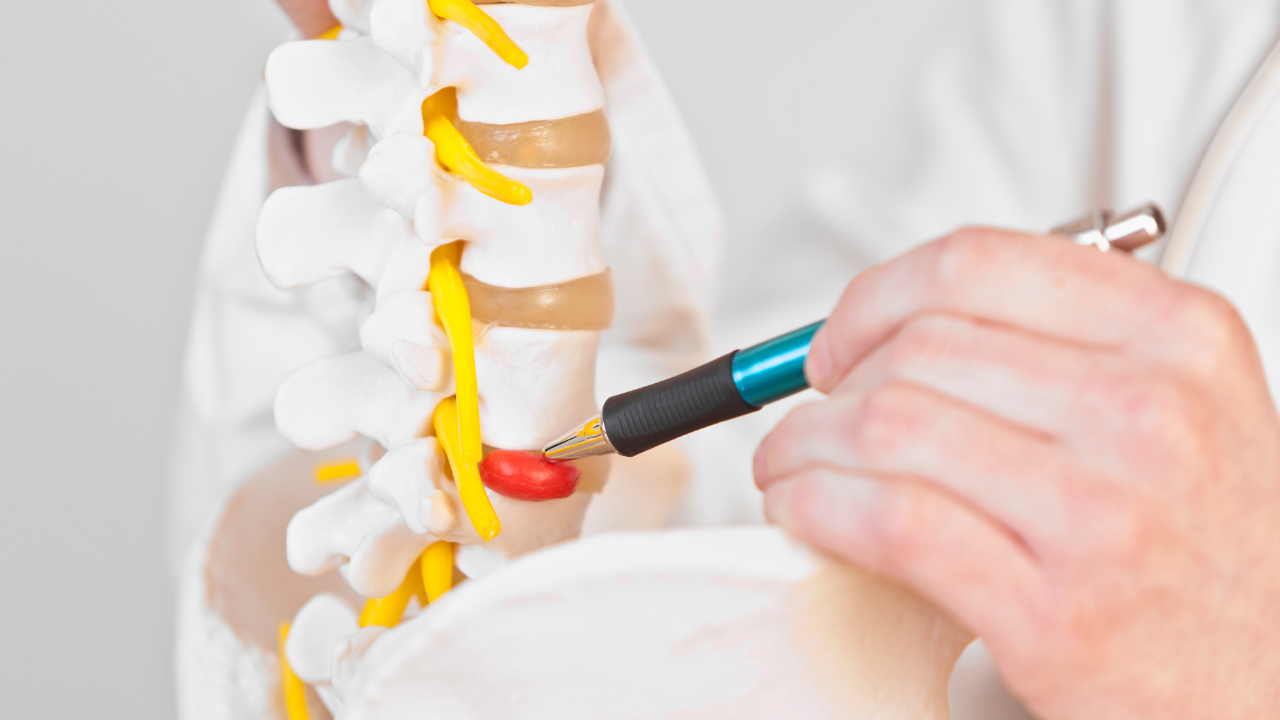
Treating Tension Type Headaches and Migraines
Trigger Point Anatomy - Epicranius Muscles
So what is the relationship between trigger points and headaches?
According to many neurologists, the most common form of headache seen in the clinic is "chronic daily headache associated with muscle tension" (chronic TTH) with periodic migrainous features.
This type of headache is often included in the category of migraine or transformed migraine, but is characterized by a background of daily headache with tender, tight muscle bands in the head, neck, and shoulder muscles (trigger points), with pain referred to the head.
A 2006 study by Calandre et al compared patients at a headache clinic, who suffered from frequent migraines, with both non-clinic subjects with fewer migraine attacks and healthy control subjects who, at most, had infrequent tension headaches.
Compelling Data
The data was compelling and indicated that trigger points can lead to both peripheral and central sensitization as well as chronic tissue changes.
These changes were directly proportional to the longevity and frequency of the migraine attacks.
Trigger Points and Migraine
Calendre investigated the presence of trigger points and elicited referred pain in 98 migraine patients and in 32 healthy subjects.
Trigger points were found in 93.9% migraines and in 29% of the control group.
The number of individual migraine trigger points varied from zero to 14, and was found to be related to both the frequency of migraine attacks, and the duration of the disease.
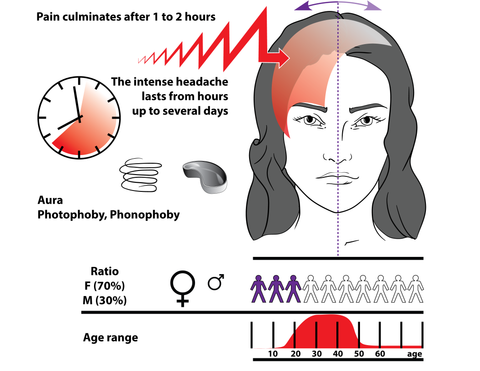
Where are the trigger points located?
About 74% of the total detected trigger points were found in the sternocleidomastoid, upper trapezius, temporalis and/or suboccipital (obliquus capitis) areas.
Other locations were mainly found in patients showing more than four trigger points such as the orbicularis occuli and occipitofrontalis.
Trigger point palpation provoked a migraine attack in 30.6% patients.
Trigger Points as "Inputs" to the Nervous System
Trigger points are also thought to be ‘input factors’ as they make their host muscle shorter and less efficient and also have a role in both peripheral and central sensitization.
This type of ‘transformed headache’ can often be reproduced by stimulating the trigger points that refer pain to the head (mainly the temporalis, obliquus capitis, sternocleidomastoid and upper trapezius).
Inactivation of the trigger points in these muscles can be an effective treatment in both the chronic and acute states.

Emotional Stimuli
Furthermore, it has been suggested that emotional stimuli may trigger the limbic system to increase muscle contractions and precipitate trigger point formation within muscles.
It is theorized that the sum of the vascular system input plus the input from trigger points and emotional stimuli determines whether or not pain is a symptom, and if so, how intense the pain is.
This could explain how some people can have trigger points or experience emotional duress without having headaches or migraines, while others get severe headaches.
People who tend to have migraines and tension headaches that occur at the same time are likely to have a very strong input from emotional factors.
Drug abuse may be another common factor.
Find a Trigger Point Professional in your area
More articles about Headaches and Trigger Points
Dry Needling for Trigger Points
Certify as a Trigger Point Therapist
About NAT Courses:
As a manual therapist or exercise professional, there is only one way to expand your business - education!
Learning more skills increases the services that you offer and provides more opportunity for specialization.
Every NAT course is designed to build on what you already know, to empower you to treat more clients and grow your practice, with a minimal investment in time and money.
Best of all, we're always here to offer help and support.

Unlimited Access to all Online Courses
NAT Education Membership Plans - $19.95/monthly
This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.

Learn More for Less
Unlimited access to all CE courses for just $19.95/mo