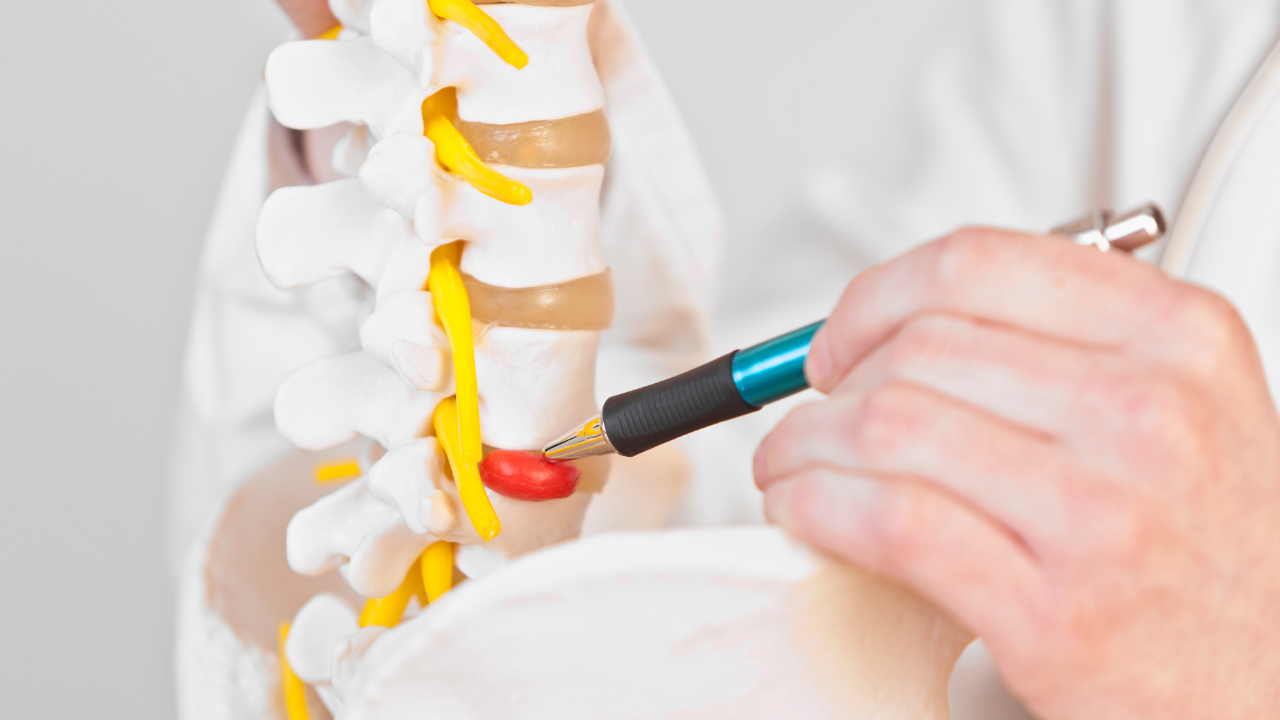
Common Causes of Chronic Lower Back Pain
Pain was once considered chronic if it lasted for more than three months and exceeded the body’s natural healing process. There has recently been significant discussion about the histological time frame of chronicity, because cells that were thought to be involved in chronic inflammation have now been found much earlier (Watson, 2015).
Chronic pain in the low back may initially result from physical structures such as:
- Disc problems
- Joint problems
- Irritation of the nerve root
But is then maintained (and on occasion made worse) by how the brain processes things. This does not mean it is all in a patient’s head; it is far too complex for that.

Image of a Herniated Disc
Lumbar herniated disc. The jelly-like center of a lumbar disc, the nucleus pulposus, herniates through the tough outer layer, the annulus fibrosus, and irritates a nearby nerve root or more likely nociceptors within the disk itself. The herniating portion of the disc is full of proteins that cause inflammation when they reach a nerve root or nerve ending. This initiates an inflammatory response and very occasionally nerve compression causing nerve root pain, although evidence suggests that the nerve can be asymptomatic even when compressed. The disc wall is also richly supplied by nerve fibers, and a tear through the wall can cause pain.
Degenerative disc disease. At birth, intervertebral discs are at their healthiest. As people age over time, discs lose hydration and wear down. Subsequently, the disc does not resist forces as well as it once did and transfers force to the disc wall—developing tears, causing pain, or weakening the annulus, leading to herniation. The disc may then collapse, contributing to spinal stenosis.
Facet joint dysfunction. There are two facet joints behind each disc at each motion segment in the lumbar spine. These joints have cartilage between the bones and are surrounded by a capsular ligament, which is richly innervated by nerves. These joints can be painful by themselves or in conjunction with disc pain.
Spinal stenosis. Pain due to narrowing of the spinal canal where the nerve roots are located. The narrowing can be central, foraminal, or both, and may be found at one level or multiple levels.
Sacroiliac joint dysfunction. The sacroiliac joint is the connection between the sacrum to each side of the pelvis. It is a strong, low-motion joint; some evidence exists to show there is no movement at this joint, and this has become an area of some contention. It primarily absorbs shock and tension between the upper body and the lower body and can become painful if inflamed (sacroiliitis) or when there is too much or too little motion of the joint.
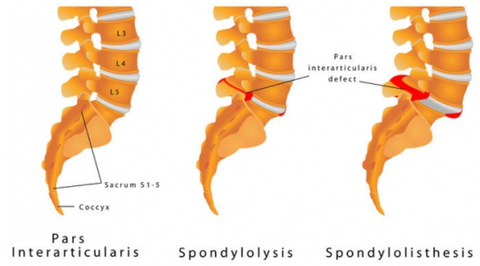
Spondylolisthesis. A condition where one vertebra slips over the adjacent one. There are 5 types of spondylolisthesis, but the most common are secondary to a defect or fracture of the pars (between the facet joints) or mechanical instability of the facet joints (degenerative). The pain arises due to the instability between the vertebrae or nerve compression.
Osteoarthritis. Wear and tear of the disc and facet joints—causing pain, inflammation, instability, and/or stenosis at these joints—occurring at one or more levels of the lumbar spine. Spinal osteoarthritis is associated with aging and is slowly progressive. It is also referred to as spondylosis or degenerative joint disease.
Deformity. Excess curvature of the spine, including scoliosis or kyphosis. These deformities may be associated with lower back pain when it leads to the breakdown of the discs, facet joints, sacroiliac joints, or stenosis.
Trauma. Lumbar back pain developing after trauma, such as a motor vehicle accidents or falls, should be medically evaluated, because they may be caused by acute fractures or dislocations of the spine.
Compression fracture. A fracture that occurs in the vertebral body whereby the bone, in effect, collapses in on itself, causing sudden pain. This type of fracture is most common due to weak bones (such as in osteoporosis) and is more common in the elderly.
It is important to note that the presence of one or more of these conditions does not necessarily mean that is the cause of pain. For example, osteoarthritis or degenerative disc disease could appear on an imaging study, but the person may not report pain.

Learn More for Less
Unlimited access to all courses for just $19.95/mo