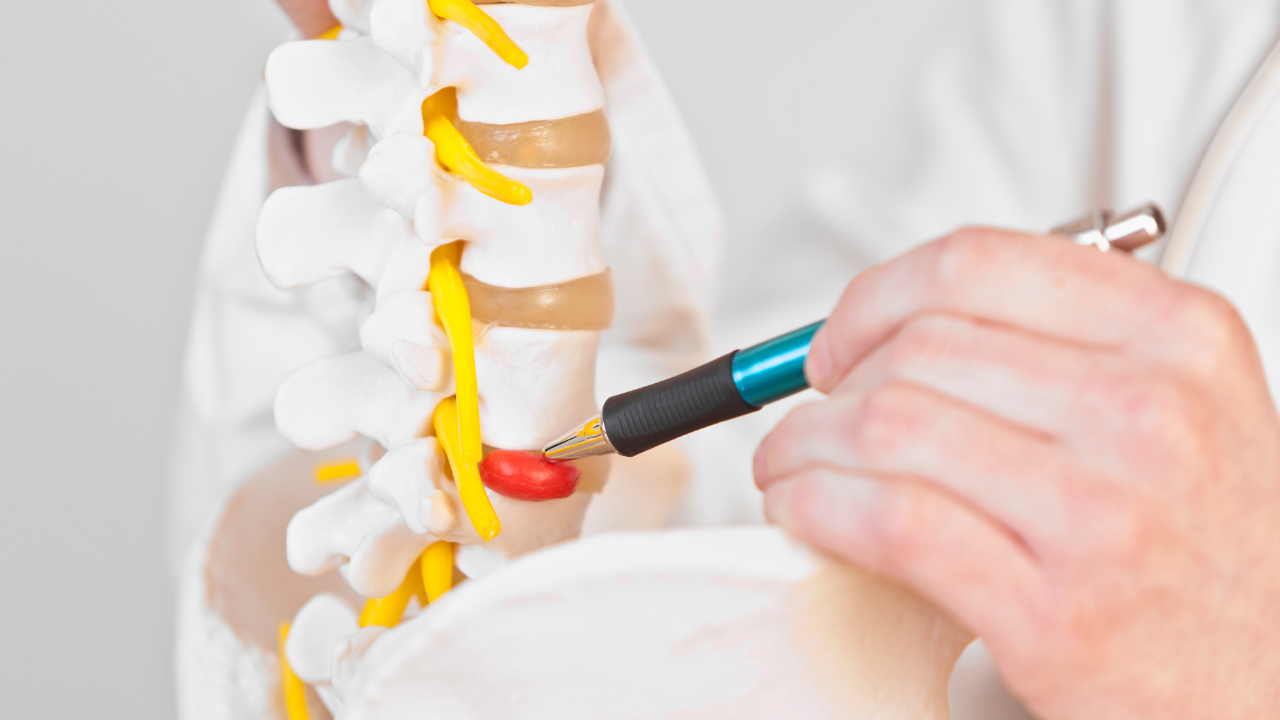
Trigger Point Therapy - Referred Pain Patterns
Referred pain is the defining symptom of a myofascial trigger point
Many of our clients come to us after receiving a diagnosis from an MD. Despite the rise in interest and use of trigger point therapy in recent years, many MD's still know little or nothing about trigger points.
This means that many clients arrive with little or no understanding of trigger points, and often have never heard of them.
We generally try to teach and inform each client about trigger points at least to the extent whereby they have a grasp of the main concepts, and can understand the details and the objectives of the treatment that they receive. I'm pretty sure that most therapists do the same.
We find that working closely with our clients in this way, seems to help accelerate the healing process.
This may be because (1) a well informed client is more likely to perform any required self help "home work" and (2) this information can help the client "visualize" their injury .... and anyone who's been doing this for a while will tell you just how powerful that can be!
Referred Pain Maps
Referred pain is probably the most important trigger point concept to discuss with clients.
Pain is a complex symptom experienced differently and individually, and referred pain is the defining symptom of a myofascial trigger point.
The client may be used to the idea of referred pain of visceral origin such as heart pain. A heart attack is often not experienced as crushing chest pain, but as pain in the left arm and hand, and in the left jaw.
This type of pain is well documented, and known to originate from the embryological dermomyotome - in this case, the heart tissue, jaw tissue, and arm tissues all develop from the same dermomyotome.

Sternocleidomastoid Muscle and Pain Map
Referred pain from a myofascial trigger point is somewhat different. It is a distinct and discrete pattern or map of pain.
This map is consistent, and has no racial or gender differences as it is the stimulation of the active trigger point that generates the pain.
The intensity of pain will vary according to the following factors (this list is not exhaustive):
- Location (attachment points are more sensitive)
- Degree of trigger point irritability
- Active or latent trigger points
- Primary or satellite trigger points
- Site of trigger point (some areas are more sensitive)Associated tissue damage
- Location/host stiffness or flexibility Aging
- Chronicity of trigger point
Clients describe referred pain as having a deep and aching quality. They also notice that movement may sometimes exacerbate symptoms, making the pain sharper.
An example of this might be a headache. In this case the client often describes a pattern of pain, or ache, which can sometimes be aggravated and made sharper by moving the head and neck.
Research Studies
A study by Kellgren in 1938 reported that pain was referred to remote locations from muscles throughout the body in response to intramuscular injection of hypertonic saline.
This gave credibility to the large series of clinical papers published independently through the following decade by three authors on three continents.
Gutstein (1938) in Europe, Kelly (1947) in Australia, and Travell (1949) in the USA reported that points of exquisite tenderness found in many muscles throughout the body were responsible for pain that projected to locations distant from the point of tenderness.
Travell and Rinzler (1952) published the first summary of the specific patterns of pain and tenderness referred from trigger points in the most commonly involved muscles throughout the body.

Infraspinatus - Trigger Points can refer pain all the way down the arm to the hand
Once upon a time we used to use illustrated books to show clients how their pain map corresponds to where the pain ought to be. This is massively helpful as well as reassuring for most clients. Nowadays we can show these pain maps on tablets or smartphones which certainly makes it even easier!
Find a Trigger Point Professional in your area
Nationally Accredited Home-Study Courses

Learn More for Less
Unlimited access to all courses for just $19.95/mo