Trigger Point Therapy - Three Dimensional (3D) Release
The agonist/antagonist relationship may not operate in the classically described manner
The brain has 3-D sensory and motor maps soft-wired into the cortex. Our brain (motor cortex) responds to our movement demands by coordinating complex sequences of motor units. These motor units can contract singly or collectively, and when more power is demanded, groups of units combine (recruitment).
One of the key ways the motor system achieves smooth coordinated movement is by utilizing the type of triangulation known as antagonism.
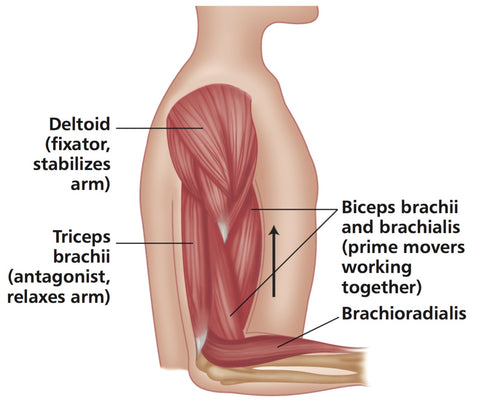
Flexion of the elbow, in which the brachialis and biceps brachii act as the agonists (prime movers), the triceps brachii as the antagonist, and the brachioradialis as the synergist.
Agonists, Antagonists, and Fixators
The triangle is formed by agonists, antagonists, and fixators (the fixators hold the joints still so that the agonist and antagonist can operate efficiently). When a trigger point develops in one of these three groups, the others are forced to compensate. That is why it is important to treat trigger points in the antagonist as well as the agonist, in other words a 3-D release.
A number of factors come into play, which magnify these effects over time. These factors are: reciprocal inhibition (where an antagonist is partially or fully switched off); pure facilitation (where an antagonist is made stronger); and co-facilitation (where increased power is routed to teams of secondary muscles).
Protective "Holding" Mechanisms
Much of the experimental data demonstrating antagonism has been generated from work with healthy volunteers. We suggest that in the pathological situation (such as a frozen shoulder), the brain is often forced to compromise this antagonism and, to this end, it exhibits a degree of neuroplasticity. In other words, the agonist/antagonist relationship may not operate in the classically described manner.
The frozen shoulder, for example, might be considered to be one of the built-in protective responses of our nervous system to avoid noxious stimuli (such as reactive tendinopathy and pain).
Every time you try to push the frozen shoulder in one direction, it pushes against you in the opposite one. The brain is constantly working to protect against what it perceives as a threat. This manifests as a stiff and painful (frozen) shoulder, with many trigger points in many muscles. (To a certain extent, we can see this protective pattern in all painful shoulder complaints).
It is as if the brain needs to take the painful shoulder (neurologically) into a “sling-like” position and hold it there for months, or even years, after the pain stimulus has remitted. This is possibly due in part to both peripheral and central sensitization.
3-D NAT Sequences
Here is an example of a basic NAT treatment for mild to moderate osteoarthritic hip (O/A hip):
-
Assess ROM.
-
Examine the muscles and note trigger points.
-
Treat trigger points in the adductors (with patient in a lateral decubitus position on the affected side), using deep stroking massage in one direction only, from the knee to the groin.
-
Use inhibition compression technique, pausing on the trigger point at the adductor insertion.
-
Turn patient onto the opposite side and treat trigger points in the TFL (deep stroking massage in a hip-to-ankle direction only) and pause on the gluteus minimus/medius trigger point using inhibition compression.
-
Articulate the hip in passive circumduction.
-
Repeat steps 4 and 5 three times.
-
Turn the patient supine and treat trigger points in the pectineus and small internal rotator hip muscles.
-
Recheck ROM.

Supine inhibition of the pectineus using the elbow.
Altered Antagonism
Having treated well over a thousand frozen shoulders, I have observed that in someone with acute shoulder pain the biceps brachii and triceps brachii pairing stops operating properly. Instead, the biceps brachii and the infraspinatus pair off; similarly, the triceps brachii and the pectoralis minor seem to change their functional relationship. NAT takes these functional antagonistic changes into account during treatment sequences.
You can observe this phenomenon for yourself. If you stimulate the trigger point in the infraspinatus somewhere near the lateral scapular border in a patient with a frozen shoulder when they are supine, they will almost always tell you that they can feel referred pain in the anterior shoulder region of the deltoid and (long head) of the biceps brachii.
In other words, treating a trigger point in the functional antagonist may reflect pain and reproduce the trigger point symptoms in the agonist.
Treat Trigger Points in Reverse
The types of functional relationship described above become apparent in particular in muscles with chronic trigger points. In such cases, it pays to establish the primary tissues that are causing symptoms and then look at the antagonistic “holding pattern.”
I have found that treating the secondary satellite or latent trigger points first, and only then the central myofascial trigger points, makes treatment more effective and longer lasting. Stimulating a sequence of three points three times (one of these points should be an STP) allows the brain to triangulate the sensory input.
The motor cortex responds by automatically releasing the holding patterns, which have become established in the 3-D map. There is an old osteopathic adage: “Treat the secondary (holding) pattern and the primary problem will sort itself out.”
Find a Trigger Point Professional in your area
More articles about Trigger Points
Trigger Point Therapy - Where to Start?
This trigger point therapy blog and the information contained in this website is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.


Learn More for Less
Unlimited access to all courses for just $19.95/mo