Trigger Point Therapy - Shoulder Arthritis
Arthritis is defined as an inflammation of one or more joints. In the case of shoulder arthritis, the symptoms are pain, and restricted range of motion, both of which may often manifest in a severe form.
Shoulder arthritis is more common than you probably think, especially in the over 50 age group. Arthritis is a growing problem as we live longer and more active lives. In fact, the most recent NHI survey in the USA found that over 60 million Americans had been diagnosed with some form of arthritis.
Whilst there is no direct cure for shoulder arthritis, manual therapy, and trigger point therapy in particular, can often help the client stay more active, and help make the symptoms way more manageable.
When treating shoulder arthritis, the very first thing we try to do, is to ensure that clients fully understand the mechanics of their shoulder as it relates to their condition. Shoulder arthritis is complex to treat, and we rely heavily on the clients involvement in terms of self managed care and adaptations of lifestyle.

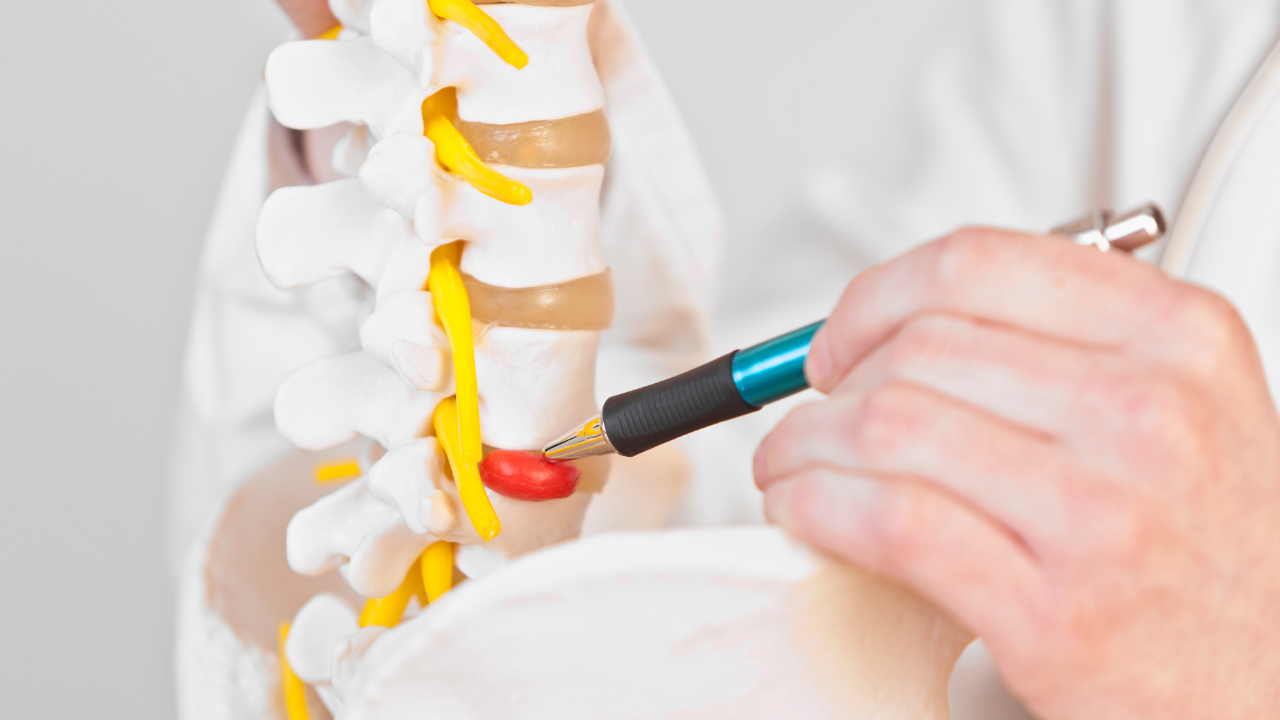
Anatomy
The shoulder is basically comprised of 3 bones. These are the Humerous (upper arm bone), Scapula (Shoulder blade), and the Clavicle (collarbone).
The shoulder is a mechanical marvel, and one that most of us take for granted. The head of the Humerous fits perfectly into a socket in the scapula. The socket is known as the Glenoid. A complex combination of muscles and tendons ensure that everything stays correctly lined-up, and operates smoothly. Together, these tissues are called the rotator cuff.
The shoulder also comprises two joints. These are the Acromioclavicular (AC) joint and the Glenohumeral joint. The first of these is positioned where the clavicle meets the tip of the shoulder blade. The second is positioned where the head of the humerus fits into the scapula.
Both of these joints may be affected by arthritis and the treatment protocols may differ considerably dependent upon which joint is affected, and the type of arthritis.
When it comes to shoulders, there are typically 5 types of arthritis:
Osteoarthritis
This is the type of arthritis that is generally described as wear and tear. Osteoarthritis attacks the smooth outer covering (articular cartilage) of the bone. The cartilage becomes diminished to the point where it becomes rough. With the wearing away of the cartilage, the required protective space between the bones decreases. Naturally this condition is made worse through day-to-day movement as the bones of the joint rub against each other. It's no wonder that Osteoarthritis causes so much pain.
This condition typically affects the 50+ age group and is more common in the Acromioclavicular joint than in the Glenohumeral joint.
Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a disease that attacks multiple joints. It is symmetrical, in the sense that it typically affects the same joint on both sides of the body.
RA is an autoimmune disease, meaning that the immune system attacks its own tissues. The defences that are there to protect us from infection instead start to attack otherwise normal tissue (ligaments, cartilage). RA causes the Synovium - which lines the joints - to swell which in turn causes the pain and restricted range of motion.
Note that RA is equally common in both shoulder joints.
Post-traumatic Arthritis
Post-traumatic arthritis is a form of osteoarthritis that develops after a trauma or injury. In the case of the shoulder, we usually see PA in clients who have previously suffered a dislocation or shoulder fracture.
Avascular Necrosis
Avascular necrosis (AVN) can be particularly nasty. AVN of the shoulder manifests when the blood supply to the head of the humerus is disrupted. Bone cells start to die and where left untreated Avascular Necrosis can eventually lead to erosion of the shoulder joint and arthritis.
AVN typically develops in stages. The dead bone slowly collapses, which in turn damages the articular cartilage and leads to arthritis. In its early stages, AVN affects the head of the humerus, but as the condition evolves, the damaged head of the humerus can in turn start to damage the Glenoid socket.
Common causes of AVN include steroid use, heavy alcohol consumption, sickle cell disease, and traumatic injury, such as a shoulder fractures. There are also instances of idiopathic AVN, meaning that no cause can be identified.
Rotator Cuff Tear Arthropathy
We see many of these cases where arthritis has developed after the client has suffered a long-term rotator cuff tendon tear. Over time and with continued activity, the torn rotator cuff becomes less able to secure the head of the humerus in the Glenoid socket. This allows the humerus to move upward and rub against the Acromion. This in turn can degrade the surfaces of the bones, and lead to arthritis.
Clients unfortunate enough to experience the combination of a large rotator cuff tear and arthritis will typically suffer sever pain and extreme stiffness, similar to the symptoms of a frozen shoulder.
What causes shoulder arthritis?
It used to be thought of as inevitable “rustiness” of getting older, simply “wear and tear” on the joints. Now experts believe it’s a lot more complicated than that, so much so that the absolute cause remains something of a mystery. We do know that there are certain factors that play a part in developing shoulder arthritis.These are:
- Previous shoulder surgery
- A car accident or similar trauma that dislocated the shoulder
- Inflammation of the shoulder (primarily due to rheumatoid arthritis
- Overuse of the shoulder
- Being over 50 – most sufferers of osteoarthritis are in the over-50 group.
- The auto-immune disease rheumatoid arthritis - this causes the body to attack and destroy its own cartilage. It wreaks havoc in different parts of the body, and can occur in the shoulder joint too
A particular “at risk” group are those who do a lot of overhead lifting activities, such as playing tennis or squash, or weightlifting.
What are the symptoms?
If you have a stiff and painful shoulder, and it hurts to move it, you may have shoulder arthritis in one form or another. Sufferers complain that it becomes more painful the more they move, and also that the pain wakes them up at night. Some people report feeling a “catching” and “grinding” or “clicking” sensation when they move. Some also say that the pain intensifies following a change in the weather.
X-Rays and MRI scans are usually the best methods of confirming a diagnosis. You should ask your doctor's advice.
Living with Shoulder Arthritis
In most cases it’s important to stick to your normal activities as much you can. Staying active stops your muscles from getting weaker. Try to keep to a properly designed exercise regime; this will help you maintain or even improve the flexibility of your joints.
Maintain a healthy weight. Excess weight puts unnecessary strain on the joints.
Try to avoid doing repetitive overhead movements that exacerbate your condition. Rest only when the joints are really painful.
Your therapist may be able to guide you through self-massage techniques that may be effective and easy to perform once you get used to them. A pressure tool might turn out to be your most effective pain killer.
Trigger Point Therapy
Whilst manual therapies do not offer a cure for any of the above forms of arthritis, there are numerous trigger Point therapy protocols that may deliver effective pain relief and significantly increased mobility.
Many of those clients who are able to access regular therapist treatments; who practice a combination of stretching and strengthening exercises between treatments; and adhere to common sense advice regarding lifestyle changes, almost always report their symptoms to become way more manageable, at the very least!
Where surgery is considered the best option, trigger point therapy can play an important part in aiding post surgical rehabilitation along with physical therapy and self managed care techniques.
Find a Trigger Point Professional in your area
Nationally Accredited Home-Study Courses
Trigger Point Master Course Collection
FREE NAT HOODIE!
$179.95
(Click to Save 20%!)
This trigger point therapy blog is intended to be used for information purposes only and is not intended to be used for medical diagnosis or treatment or to substitute for a medical diagnosis and/or treatment rendered or prescribed by a physician or competent healthcare professional. This information is designed as educational material, but should not be taken as a recommendation for treatment of any particular person or patient. Always consult your physician if you think you need treatment or if you feel unwell.

Learn More for Less
Unlimited access to all courses for just $19.95/mo